At the Jack & Sheryl Morris Cancer Center, our approach to cancer care centers on treating the individual, not just the illness. Our multidisciplinary Gastrointestinal Cancer team includes nationally recognized experts in surgical oncology, gastroenterology, medical oncology, and supportive services who work collaboratively to design customized treatment plans. Whether you’re facing a new diagnosis or exploring a second opinion, we are committed to guiding you with expertise, compassion, and reassurance at every stage.
What Are Esophageal and Gastroesophageal Junction Cancers?
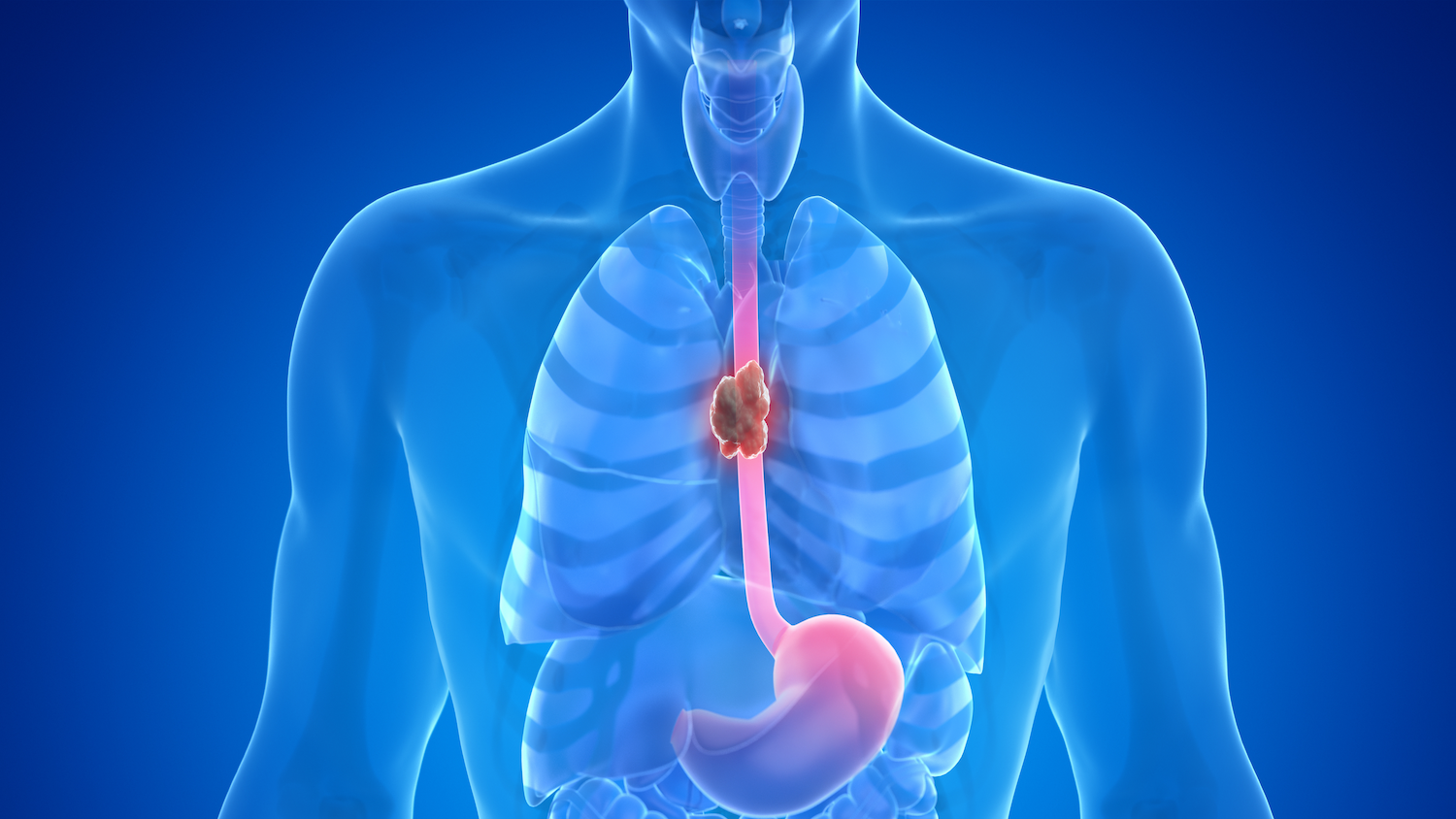
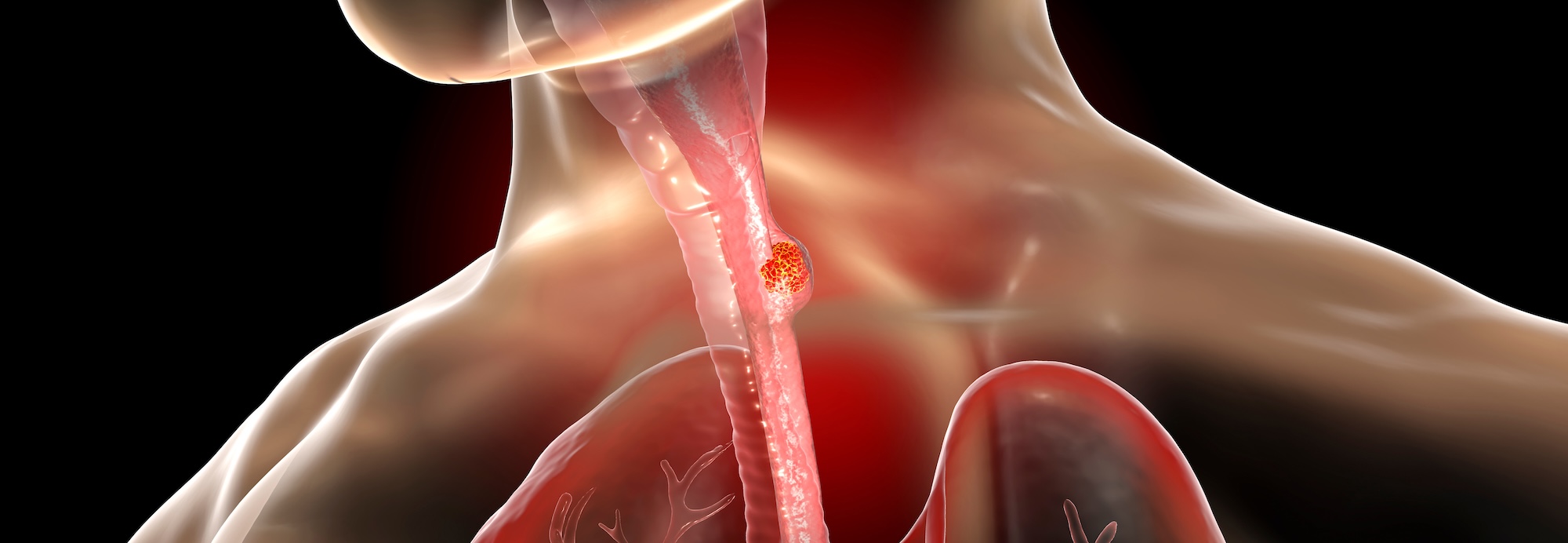
Esophageal cancer begins in the lining of the esophagus — the tube that carries food from the throat to the stomach.
Gastroesophageal junction (GEJ) cancer starts where the esophagus meets the upper part of the stomach. These two areas are closely related, and their cancers often share similar causes, symptoms, and treatments.
There are two main types:
- Adenocarcinoma, usually found in the lower esophagus or GEJ, often related to chronic acid reflux or a condition called Barrett’s esophagus.
- Squamous cell carcinoma, which tends to occur in the upper or middle esophagus and is more strongly associated with tobacco and alcohol use.
Because early-stage disease may cause few or no symptoms, these cancers are often detected later — which is why early recognition and surveillance for those at risk are critical.
Signs & Symptoms of Esophageal and Gastroesophageal Junction Cancers
Symptoms can differ depending on where the cancer forms and how advanced it is.
Common signs include:
- Difficulty or pain when swallowing
- Feeling like food sticks in the chest or throat
- Unexplained weight loss
- Persistent heartburn or reflux
- Chest pain or pressure
- Hoarseness, chronic cough, or sore throat
- Fatigue or weakness
If you experience trouble swallowing or reflux that doesn’t improve with medication, speak with your doctor. Early evaluation can lead to earlier detection and better outcomes.
How Are Esophageal and Gastroesophageal Junction Cancers Diagnosed?
Diagnosis begins with a detailed evaluation of symptoms, medical history, and risk factors. Tests may include:
- Upper endoscopy (EGD): A thin, flexible scope allows doctors to view the esophagus and stomach and take biopsies.
- Imaging studies: CT, PET, or endoscopic ultrasound to determine tumor size, depth, and spread.
- Pathology review: Expert gastrointestinal pathologists examine tissue to define cancer type and stage.
- Molecular testing: Advanced tests identify genetic and molecular markers that can guide targeted or immunotherapy treatments.
At the Jack & Sheryl Morris Cancer Center, all imaging and pathology are reviewed by subspecialists in gastrointestinal cancers, ensuring the most accurate and complete diagnosis.
Available Treatment Options for Esophageal and Gastroesophageal Junction Cancers
Each treatment plan is personalized and guided by a team of specialists working together to provide the most effective and compassionate care. Depending on your diagnosis, treatment may include surgery—often using minimally invasive or organ-sparing techniques—along with chemotherapy, targeted therapy, immunotherapy, or radiation therapy to destroy cancer cells and prevent recurrence.
As part of an NCI-designated Comprehensive Cancer Center, our patients also have access to innovative clinical trials offering promising new therapies. Throughout your care, our team provides comprehensive supportive services — including nutrition, rehabilitation, and emotional support — to help you heal, recover, and live fully beyond cancer.
Gastrointestinal Surgery and Advanced Procedures
Our surgical oncologists specialize in minimally invasive and robotic gastrectomy, offering faster recovery, less pain, and improved long-term function. When appropriate, we perform organ-sparing and endoscopic resections for early-stage cancers to preserve normal digestion. Each operation is planned collaboratively with nutrition, anesthesia, and recovery specialists through our enhanced recovery pathways, which support patients before and after surgery.
Systemic and Precision Therapies
Our medical oncologists tailor treatment using the latest targeted and immunotherapy agents, designed to exploit specific tumor features such as HER2, PD-L1, or CLDN18.2. These cutting-edge therapies — often combined with chemotherapy — are changing outcomes for patients with both localized and advanced gastric cancers. As part of an NCI-designated Comprehensive Cancer Center, our patients also have access to clinical trials exploring next-generation immunotherapy, molecular diagnostics, and precision-based drug development.
Radiation and Chemoradiation
For select patients, chemoradiation may be used to shrink tumors before surgery or treat disease that cannot be removed surgically. Our radiation oncology team uses advanced technologies such as intensity-modulated radiation therapy (IMRT) and image-guided radiation therapy (IGRT) to deliver radiation exactly where it’s needed, protecting nearby organs like the heart and lungs. In select cases, proton therapy may be an option. Our radiation oncology experts will help determine whether it offers meaningful benefit compared with standard photon therapy.
Clinical Trials and Research
As a leader in cancer research, the Jack & Sheryl Morris Cancer Center provides patients with access to innovative clinical trials exploring new treatments for stomach cancers. Our investigators are studying novel combinations of chemotherapy, targeted agents, immunotherapies, and minimally invasive surgical techniques designed to improve survival and quality of life. Participating in a clinical trial may offer access to tomorrow’s breakthroughs today — while helping advance discoveries that benefit future patients.
You can explore currently available studies and search by diagnosis, treatment type, or keyword using our Clinical Trials Search Portal.
For personalized assistance, contact our research team to connect with a coordinator who can help identify trials that may be right for you.
Additional Treatments
- Support for patients living with cancer through the Survivorship Program
Meet Our Team
Surgical Oncologists
H. Richard Alexander, Jr., MD, FACS
Chief Surgical Officer,
Chief, Surgical Oncology, Rutgers Cancer Institute;
System Director of Surgical Oncology, RWJBarnabas Health;
Surgeon-in-Chief of the Jack & Sheryl Morris Cancer Center
Haejin In, MD, MPH, MBA, FACS, FSSO
Chief Strategic Excellence and Engagement Officer
Associate Director of Strategic Excellence and Engagement
Surgical Oncologist
Mariam Eskander, MD, MPH
Surgical Oncologist
Assistant Professor in the Department of Surgery, Rutgers Robert Wood Johnson Medical School
Medical Oncologists
Stacey Stein, MD
Medical Oncologist
Medical Oncology Director for Hepatobiliary Cancer, RWJBarnabas Health
Prateek Gulhati, MD, PhD
Associate Director for Clinical Research and Director, GI Oncology, Rutgers Cancer Institute
Director of Oncology Research, RWJBarnabas Health
Radiation Oncologists
Salma Jabbour, MD
Radiation Oncologist
Clinical Chief, Radiation Oncology at RWJUH & Rutgers Cancer Institute
Associate Director for Faculty Affairs and Development
Vice Chair of Clinical Research & Faculty Development
Matthew Pierre Deek, MD
Radiation Oncologist
Assistant Professor, Division of Clinical Radiation Oncology
Thoracic Surgeons
Ioannis Kontopidis, MD
Thoracic Surgeon
Assistant Professor of Surgery, Rutgers Robert Wood Johnson Medical School
Advanced Gastroenterology
Radiology (Gastrointestinal Cancer Specialists)
Our Multidisciplinary, Patient-Centered Approach
Every patient we see benefits from the collective expertise of a multidisciplinary care team dedicated to delivering coordinated, individualized, and compassionate care. From the moment you arrive, your case is reviewed by surgical oncologists, medical and radiation oncologists, gastroenterologists, pathologists, radiologists, dietitians, and supportive care specialists. Together, they develop a treatment plan tailored specifically to your diagnosis, health goals, and personal needs. This collaborative model ensures you receive the most advanced, evidence-based care available — combining the strengths of every specialty under one roof. Your team meets regularly to review progress, adjust plans, and ensure that each decision reflects the latest research and your evolving goals.
What sets our program apart:
- Expertise and Experience: Nationally recognized leaders in gastric and esophageal cancer care, skilled in complex and minimally invasive procedures.
- Innovation in Care: As part of an NCI-designated Comprehensive Cancer Center, we offer access to cutting-edge clinical trials and translational research that bring new therapies directly to patients.
- Seamless Coordination: Dedicated nurse navigators guide you through scheduling, testing, and consultations — so you can focus on healing, not logistics.
- Whole-Person Support: Our team provides nutrition counseling, rehabilitation, psychological support, and survivorship services to help you live fully during and after treatment.
At the Morris Cancer Center, our mission goes beyond curing disease — it’s about restoring health, dignity, and hope. Every member of your care team is here not only to treat your cancer, but to walk with you through every phase of your journey.
Additional Resources
Related Articles and Press
Answers from an Expert: Esophageal Cancer
Benjamin Medina, MD, thoracic surgeon in the Lung/Thoracic Oncology Program at Rutgers Cancer Institute of New Jersey and RWJBarnabas Health, answers common questions about esophageal cancer.